In a previous post, we introduced the Neuropathy Tracker and its publication in PLOS Digital Health, describing how a smartphone-based application can support ambulatory, self-administered assessment of neuropathy [1].
The Neuropathy Tracker has now undergone clinical validation in a recent study published in BMJ Neurology Open [2]. This study provides important evidence that patient-administered, smartphone-based assessment can align closely with established clinical evaluation methods.
This marks an important step—not only for the Neuropathy Tracker itself, but also for CARP’s broader vision as a foundation for building clinically valid digital health solutions.
The Challenge: Scalable Assessment of Neuropathy
Distal symmetrical peripheral neuropathy (DSPN) is a common condition that requires repeated clinical evaluation to monitor symptoms and progression. These assessments are essential for diagnosis, classification, and treatment planning—but they are also resource-intensive and burdensome for both patients and healthcare systems.
Traditionally, evaluation relies on in-person clinical examinations performed by trained professionals using validated scoring systems such as:
- Utah Early Neuropathy Scale (UENS)
- Total Neuropathy Score – Clinical Version (TNSc)
This raises a fundamental question:
Can patients reliably perform parts of this evaluation themselves—outside the clinic?
The Study: Comparing Self-Assessment with Clinical Evaluation
The study included 21 patients with neuropathy and 18 control participants and compared:
- Neuropathy Tracker (patient self-assessment via smartphone)
- UENS and TNSc (clinical gold-standard assessments)
- Supporting laboratory measures (QST and nerve conduction studies)
A key strength of the study is its test–retest design, allowing for a robust evaluation of reliability, as well as blinded comparison between patient-administered and clinician-administered assessments.
The Neuropathy Tracker guides patients through a structured, step-by-step evaluation of symptoms and signs—including sensory testing, vibration perception, and motor function—using only a smartphone.
Key Findings
Reliable and Comparable to Clinical Assessment – The Neuropathy Tracker showed no significant bias when compared to the UENS scale and demonstrated similar variability in repeated measurements. Correlation between repeated self-assessments was high (r ≈ 0.92), indicating strong reliability.
Strong Diagnostic Performance – The app demonstrated excellent ability to classify neuropathy, with an area under the curve (AUC) of approximately 0.90 (see Figure 1). While slightly below clinician-administered tools, this level of performance is notable given that assessments were performed independently by patients.
Independent Use by Patients – Participants were able to complete the assessment on their own, without supervision, highlighting the feasibility of at-home clinical evaluation.
The study also shows that while the Neuropathy Tracker aligns well with UENS, it is not directly interchangeable with TNSc, reflecting differences in how these scales capture neuropathy.
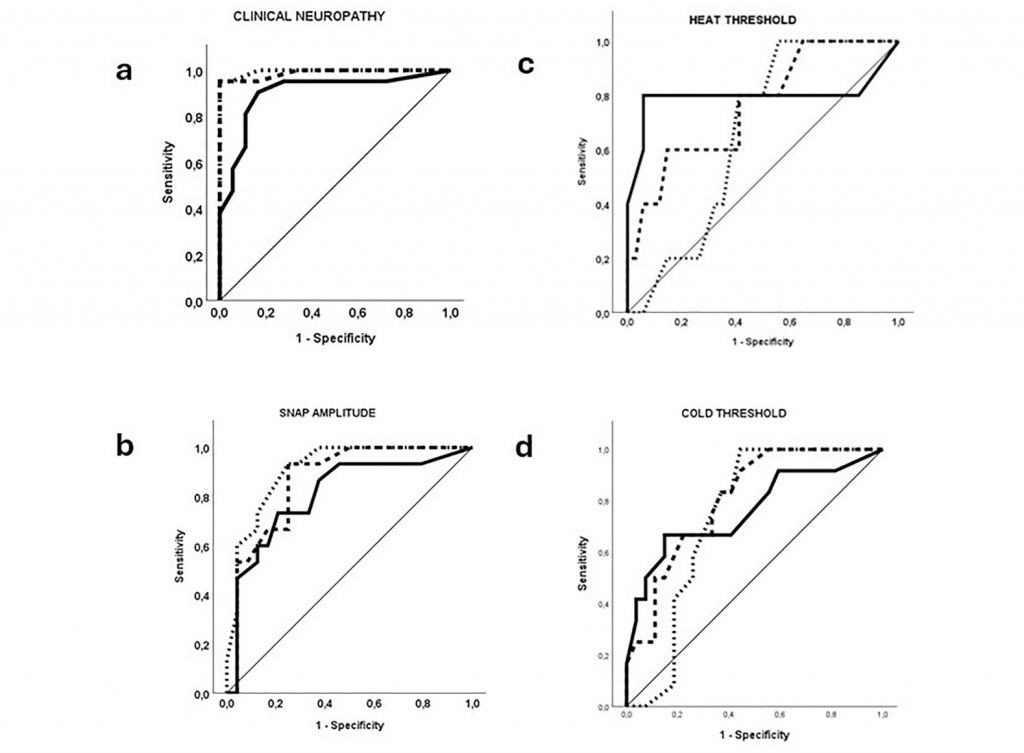
Early Neuropathy Scale (stippled line) and Total Neuropathy Score Clinical (punctate line). The state definitions for discriminating
between normal and abnormal are either (a) clinical neuropathy, (b) Sensory Nerve Action Potential (SNAP) Amplitude, (c) warm
detection threshold (WDT, HEAT in the figure), or (d) cold detection threshold (CDT, COLD in the figure). For (b)–(c), the level
of abnormality is at ±2 SD from the age- corrected mean of reference data. The line of reference represents the limit for no
diagnostic ability.
What This Means for Clinical Practice
The results suggest that smartphone-based self-assessment can play a meaningful role in clinical workflows.
Specifically, the Neuropathy Tracker can:
- Supplement clinical evaluations between visits
- Enable remote monitoring of disease progression
- Support earlier detection and triaging
- Reduce the need for unnecessary in-person consultations
Importantly, the study highlights that patient-generated data can provide valid and clinically relevant information, even outside traditional healthcare settings.
Linking Back to CARP: From Framework to Clinical Evidence
The Neuropathy Tracker is built using CARP Flutter components, which provide the underlying infrastructure for:
- Defining structured clinical assessment protocols
- Guiding users through complex evaluation workflows
- Collecting high-quality, reproducible data
It demonstrates that CARP can be used to build digital health tools that are clinically valid. This is a crucial step in moving from isolated mHealth apps to a systematic, reusable, and evidence-based digital health platform.
Towards Scalable Digital Health
The implications extend beyond neuropathy.
A CARP-based approach enables the development of similar tools for:
- Chronic disease monitoring
- Cognitive and neurological assessment
- Digital phenotyping in large-scale studies
- Decentralized and hybrid clinical trials
By combining structured protocols, mobile sensing, and guided interaction, CARP supports a new generation of digital health applications that can operate both inside and outside the clinic.
Wrapping Up
The clinical validation of the Neuropathy Tracker marks an important milestone. It shows that:
- Patients can perform meaningful clinical assessments themselves
- Smartphone-based tools can align with established clinical methods
- CARP provides a viable foundation for building such tools
More broadly, it reflects a shift towards patient-centered, scalable, and data-driven healthcare, where validated digital tools extend clinical insight beyond the walls of the hospital.
Reference
- Bardram JE, Westermann M, Makulec JG, Ballegaard M (2025) The Neuropathy Tracker—A mobile health application for ambulatory and self-administred assessment of neuropathy. PLOS Digital Health 4(2): e0000725. https://doi.org/10.1371/journal.pdig.0000725
- Madsen AEK, Haverberg MJN, Bardram JE, Ballegaard M. Smartphone-based patient self-assessment of neuropathy grade: a validation study of the Neuropathy Tracker alignment with clinical tests. BMJ Neurology Open, 2025.